December 27, 2021

Nov 04, 2025

Oct 14, 2025

Dec 20, 2022

Jul 21, 2022

Jul 29, 2020

Nov 04, 2025

Oct 14, 2025

Dec 20, 2022

Jul 21, 2022

Jul 29, 2020
April 01, 2021

In what appears to be the first Pennsylvania State Court ruling which addresses in detail the “physical loss of or damage to” hurdle for COVID-19 business interruption claims in property policies, the Court of Common Pleas in Allegheny County granted summary judgement in favor of a dental practice which was required to close most of its business due to the governor’s stay at home orders.
Judge Christine Ward rejected CNA Insurance Company’s argument that “direct physical loss of or damage to property” requires some physical alteration of or demonstrable harm to the policyholder’s property. In so holding, the Court declined to follow the interpretation of most of the state and federal courts that the term “direct physical loss of or damage to property” requires some form of physical altercation and/or harm to property in order for the insured to be entitled to coverage.
Instead, Judge Ward reasoned that “any such interpretation improperly conflates ‘direct physical loss of’ with ‘direct physical…damage to’ and ignores the fact that these two phrases are separated in the policy by the disjunctive ‘or’” which requires the Court to conclude that “direct physical loss of” must mean something different than “direct physical…damage to.”
For similar reasons, the Court also rejected CNA’s objections to coverage under the Civil Authority coverage of the Policy, which provides coverage for business income losses caused by an action of civil authority that prohibits access to the insured property. The Court held that the orders issued by the state government to mitigate the spread of COVID-19 “effectively prevented…citizens of the Commonwealth from accessing Plaintiff’s business in any meaningful way for normal, non-emergency procedures”, dismissing CNA’s argument that complete prohibition of access to the property would be required for coverage to be triggered.
Lastly, the Court considered CNA’s position that the “contamination” and/or the “fungi, wet rot, dry rot and microbes” exclusions precluded coverage for the Plaintiff’s claim. In rejecting the application of the contamination exclusion, the Court noted that “the cause for the loss of use of property [for Plaintiff] was not the contamination of property” but rather “the risk of person-to-person transmission of COVID-19, which necessitated social distancing measures and fundamentally changed the way businesses utilized physical space” (emphasis in original).
In holding that the “microbes” exclusion did not apply to Plaintiff’s claim, the Court engaged in a fairly lengthy discussion about the similarities and differences between the definition(s) of what constitutes a “microbe” and “virus”, but ultimately concluded that given the ambiguity present in the use of the undefined term “microbes” in the Policy, the Court must find in favor of the Plaintiff.
The question now becomes, what, if any, impact this decision will have for policyholders in Pennsylvania and beyond. The Court may have come out differently in the event the Policy in question had a well-defined virus exclusion. Over the years insurance carriers have used various virus exclusion provisions in their policy forms. How each exclusion will be interpreted and applied by the courts has yet to be seen.
One thing is certain, CNA will undoubtedly appeal this decision and advocate for a different outcome in the appellate court(s). From a statistical perspective, the odds appear to be in CNA’s favor. According to the University of Pennsylvania School of Law’s COVID Litigation Tracker, over 1,500 cases have been filed in state and federal courts throughout the country, fighting carriers for coverage for business income losses sustained as a result of the global pandemic. Of those that have been decided by the courts, an overwhelming majority of them have been decided in favor of the insurance carrier by either denying the motion or issuing a full dismissal. Obtaining coverage for COVID-19 business interruption losses will still be unlikely since most property policies included an explicit virus exclusion. Your Graham Company Claims Consultant will continue to monitor this case and advocate on your behalf if there is a potential to trigger coverage based on the wording in your property policy.

Nov 04, 2025

Oct 14, 2025

Feb 21, 2023

Jul 21, 2022

Dec 14, 2021
March 30, 2021

OSHA has published statistics on their response to the COVID-19 Pandemic. According to the OSHA COVID-19 Response summary, between February 1, 2020 and March 7, 2021 Federal OSHA has received at total of 16,025 complaints and referrals. These are typically the events that trigger an OSHA inspection. Of these 16,025 triggering events, OSHA has opened inspections for 1,771 of these complaints and referrals.

Federal OSHA Enforcement Updates
OSHA has recently posted the most common citations issued related to COVID-19. Citations have focused heavily on violation of the Respiratory Protection Standard (29 CFR 1910.134) and to a lesser extent on the OSHA Recordkeeping standard (29 CFR 1904). Along with the most common citations, OSHA included guidance documents and other resources to assist employers with compliance. These inspections have produced citations at 310 of the facilities as of January 14, 2021.

Recordkeeping and Reporting Citations:

COVID-19 related OSHA Inspections by the numbers
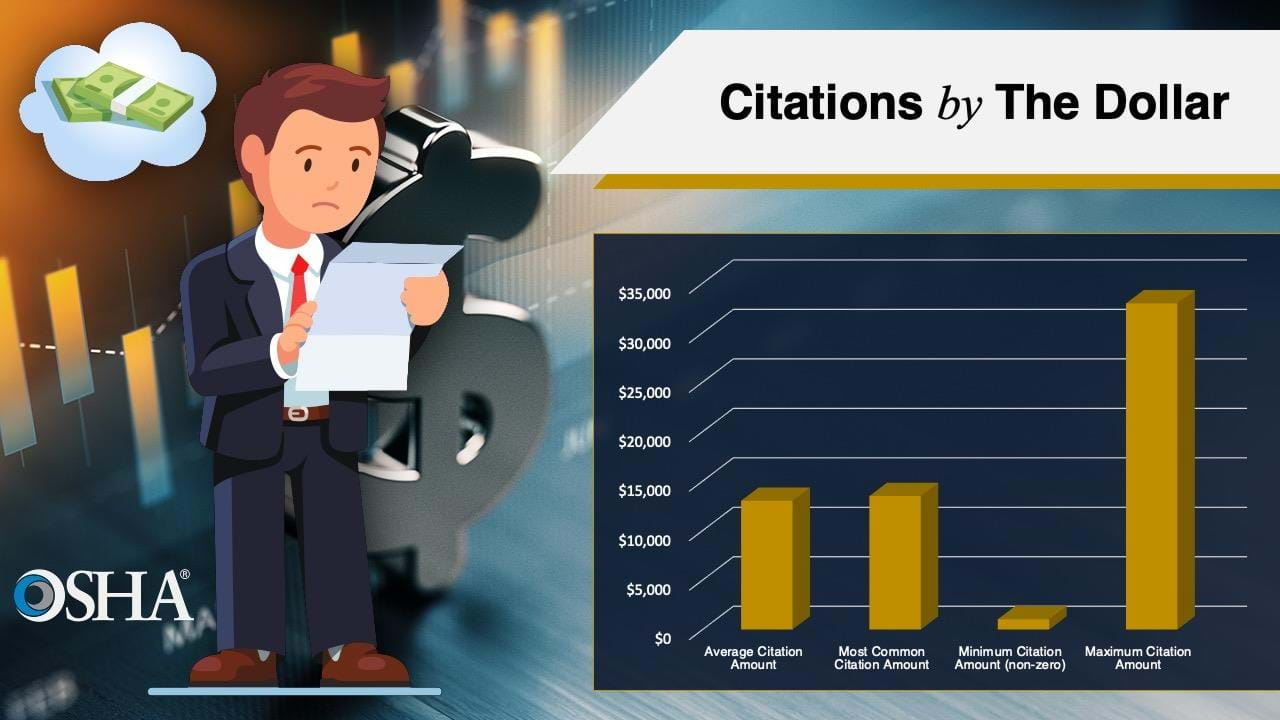
Citations by the Dollar
Employers are advised to evaluate the use of Respirators and to implement a comprehensive Respiratory Protection Program if respirators are required.
Employers should also ensure they are making correct decisions on OSHA Recordkeeping and Reporting. Refer to the chart below for information on when to report a work-related fatality or inpatient hospitalization. Refer to the OSHA’s Revised Enforcement Guidelines for Recording Cases of COVID-19.
|
Type of Incidents Related to COVID-19 |
Reporting Requirement |
|
Work-related fatality |
Report to OSHA within 8 hours (if the fatality occurs within 30 days of incident or last exposure) |
|
Work-related in-patient hospitalization of one or more employees |
Report to OSHA within 24 hours (if the hospitalization occurs within 24 hours of incident or last exposure) |
|
Work-related amputation or loss of an eye |
Report to OSHA within 24 hours (if the amputation or loss of eye occurs within 24 hours of the incident) |
If you have any questions on this increase in COVID-related complaints and inspections and how this may impact your organization, please contact your Graham Company Safety Consultant.

Nov 04, 2025

Oct 14, 2025

Jul 21, 2022

Feb 23, 2023
January 12, 2021

The final quarter of 2020 was perhaps the most “normal” with respect to all issues compliance- and benefits-related. We saw the typical updates of federal limits for various benefits/fees and some additional guidance around various Covid-19 related benefits issues. One surprise was perhaps the Covid-19 relief bill signed by President Trump just last week, which provided additional relief for Section 125 health flexible spending arrangements and Section 129 dependent care assistance programs. You can read more about these changes, along with other significant regulatory news, below.
Many of us assumed that the National Emergency would not end on April 30th, 2020 as the agency guidance suggested in its examples, however, we all hoped it would be over by now. As the National Emergency continues, more employers find themselves having to deal with late COBRA elections and payments, enrollment requests well beyond the typical 30-day window, and a seemingly never-ending run-out period for HRAs and health FSAs.
As a quick reminder, last April the agencies issued a joint final rule extending time frames for COBRA elections and payments, HIPAA special enrollment notices, and ERISA claim submissions. The rule indicated that all applicable deadlines were suspended beginning March 1st, 2020 until 60 days after the end of the National Emergency (i.e. the “Outbreak Period”). President Trump has not declared the National Emergency over, and Congress hasn’t taken any such action either, so the Outbreak Period continues without any definite end in sight. Over a short period of time, the Outbreak Period certainly provided some additional protection and flexibility for employees while having only a minor impact on employers and plan administration. However, as the Outbreak Period drags on, the burden for employers has increased.
COBRA
The biggest struggle and risk to employers is likely the extended COBRA election and payment deadlines.
The employer must carefully coordinate this decision with the carrier (or stop-loss vendor) to ensure the carrier will provide coverage, suspend claims, or terminate/reinstate retroactively. In addition, the employer should really make this decision uniformly for all COBRA participants and ensure the COBRA administrator will handle administration accordingly. Unless the COBRA participant confirms a desire to discontinue coverage (beyond just failing to pay), the employer must ensure there is a way to provide the coverage if the individual eventually makes payment.
HIPAA Special Enrollments
Many employers have struggled over the last couple months with HIPAA special enrollment requests as well. Employees who request mid-year enrollment due to a loss of coverage, acquisition of a dependent due to marriage or birth/adoption, or becoming newly eligible for a Medicaid/CHIP subsidy are generally required to request enrollment within 30 or 60 days of the event depending upon which event occurred. This 30-day (or 60-day) notification period is suspended during the Outbreak Period, meaning an event could occur now and enrollment could be requested up until 30 (or 60) days following the end of the Outbreak Period. NOTE: The extension applies to the notice timeframe, but does not change the requirements for the effective date. Upon receiving a request for enrollment, the plan is in compliance so long as coverage is made effective no later than 1st of the month following receipt of the notice, unless the triggering event was a birth or adoption, in which case the plan must make coverage effective retroactively back to the date of birth or adoption.
For example, if an employee got married in September 2020, a HIPAA special enrollment right is triggered for the employee, spouse and any newly acquired dependents (e.g. stepchildren).
Typically notice of the event would be required within 30 days of the marriage for any such individuals to exercise their special enrollment right. However, if the employee requested enrollment for the spouse in December 2020, the plan would be in compliance so long as coverage for the spouse was made effective no later than January 1st, 2021.
HRA and Health FSA Claims
While the agencies’ joint rule doesn’t specifically address health FSA or HRA claims, it is generally accepted that because claims for reimbursement under a health FSA or HRA are considered “ERISA claims” they are therefore subject to the extended deadlines during the Outbreak Period. For a health FSA or HRA, rather than submission within a date tied to when each expense was incurred, claims are generally required to be submitted within a certain time frame following the end of the plan year (i.e. a run-out period). If a 2019 plan year’s run-out period extended beyond March 1st, 2020, it appears that the employer would have to allow claims incurred during the 2019 plan year to be submitted for reimbursement through the end of the Outbreak Period + any time that was remaining in the run-out period as of March 1st, 2020. As time passes, it becomes less likely that plan participants are still holding onto claims for reimbursement from a 2019 plan year that ended early in 2020. However, employers with plan years that ended in the second half of 2020 should keep this requirement in mind as their normal run-out periods end and the Outbreak Period continues.
In Other News… Recap of 4th Quarter Issue Briefs and Alerts
2020 Employer Reporting – Slight Extension & Transition Relief
IRS Notice 2020-76 once again extends the due date to March 2nd, 2021 for providing Form 1095s to individuals and is allowing Form 1095-Bs to be made available upon request rather than requiring individual delivery. The IRS also granted one final year of penalty relief for good faith reporting errors.
More here: https://benefitcomply.com/2020-employer-reporting-slight-extension-transition-relief/
IRS Announces 2021 Health FSA & Qualified Transportation Limits
In Revenue Procedure 2020-45, the IRS sets forth a variety of 2021 adjusted tax limits. Among other things, the notice indicates that employee contribution limits toward health flexible spending arrangements (FSAs) and qualified transportation fringe benefits are unchanged for 2021. The limit on annual employee contributions toward health FSAs for 2021 is $2,750, with the ability to carryover up to $550. (And note that the recently-passed Covid-19 relief legislation mentioned below temporarily increases the carryover to an unlimited amount.) The limit on monthly contributions toward qualified transportation and parking benefits for 2021 remains at $270.
More here: https://benefitcomply.com/irs-announces-2021-health-fsa-qualified-transportation-limits/
Schedules A & C: A Closer Look
Schedules A & C are attached to Form 5500 and used to report insurance and service provider information, respectively. In this issue brief, we briefly discuss the basics of each schedule, clear up some common misconceptions surrounding the schedules, and provide a few tips for Form 5500 preparers. Finally, we preview proposed 5500 reporting changes.
More here: https://benefitcomply.com/schedules-a-c-a-closer-look/
Updated PCORI Fees Released
In Notice 2020-84, the IRS provided the adjusted PCORI fee of $2.66 for plan years ending in October 2020 through September 2021. Employers who sponsored self-funded group medical plans are required to report and pay the ACA Patient-Centered Outcomes Research Institute (PCORI) fees annually. In the spending bill passed late in 2019, the PCORI fee (which was set to expire) was extended another 10 years.
More here: https://benefitcomply.com/updated-pcori-fees-released/
Group Health Plan Coverage of COVID-19 Immunizations
Non-grandfathered group health plans must prepare to provide coverage for COVID-19 immunizations with no cost-sharing. Coverage with no cost-sharing must be available for both in-network and out-of-network providers within 15 days of such immunizations being recommended by the United States Preventive Services Task Force (USPSTF) or the Advisory Committee on Immunization Practices (ACIP). Grandfathered group health plans are encouraged, but not required, to provide this coverage as well.
More here: https://benefitcomply.com/group-health-plan-coverage-of-covid-19-immunizations/
Health & Welfare Benefit Nondiscrimination Rules
Employers are generally permitted to structure plans with different eligibility, benefits, and contributions between classes of employees so long as the employer does not discriminate against a protected class (e.g., age, disability, race, religion, or sex) or based on health status. However, to offer benefits on a tax-favored basis, plans must be structured in accordance with benefit nondiscrimination rules. Benefit nondiscrimination rules restrict the ability to favor highly compensated individuals or key employees on a tax-favored basis. Benefit nondiscrimination rules are enforced by the IRS. Failure to comply with benefit nondiscrimination rules risks the highly compensated and key employees being taxed on benefits received under the discriminatory plan.
More here: https://benefitcomply.com/health-welfare-benefit-nondiscrimination-rules/
Can Employers Require COVID-19 Vaccinations?
As COVID-19 vaccines become available, many employers will have a strong case for requiring employee vaccinations, so long as their vaccination policies have certain exceptions, are job-related, and are consistent with business necessity, legal experts say…
Important Note: This alert provided by Guardian HR Compliance, a Benefit Comply service. For more information on employer HR compliance support please visit https://benefitcomply.com/hr-support
More here: https://benefitcomply.com/can-employers-require-covid-19-vaccinations/
Significant Benefits Issues in New COVID-19 Relief Legislation
The recently passed COVID-19 relief legislation contains some important benefits-related provisions. We have drafted two different compliance alerts outlining key provisions. The first provides a high-level overview of the most important benefits provisions in the legislation, including new flexibility regarding Section 125 and 129 reimbursements and elections. The second is a more detailed dive into the 125 and 129 changes.
More here: https://benefitcomply.com/significant-benefits-issues-in-new-covid-19-relief-legislation/

Nov 04, 2025

Oct 14, 2025
December 16, 2019
In this issue, our Vice Chairman Michael Mitchell discusses how Graham Company is embracing innovation to transform business operations. Given the rapidly evolving threat landscape, Vice President Nicholas Cushmore explains the importance of cyber insurance and what to do in an event of a cyberattack.

Nov 04, 2025

Oct 14, 2025

Jan 24, 2022

Nov 10, 2021
August 14, 2019
In this issue, Bill Graham discusses the impetus for Graham’s unique hiring process. The Graham team that works with Allan Myers highlights their role in providing 24/7 strategic counsel.

Nov 04, 2025

Oct 14, 2025

Jan 24, 2022

Nov 10, 2021
April 18, 2019
In this issue, Mike Mitchell discusses upcoming neurodiversity event. The Graham team that works with SSH Real Estate weighs in on a disaster recovery situation.

Nov 04, 2025

Oct 14, 2025
December 17, 2018
In this issue, Mike Mitchell provides an update on cybersecurity regulations. The Graham team that works with Merakey discusses the success behind the 20-year partnership.

Nov 04, 2025

Oct 14, 2025

Jul 21, 2022

Jul 29, 2020
August 08, 2018
In this issue, Ken Ewell discusses the growth of Graham Company and a recent honor bestowed upon Bill Graham. Tom Morrin, in collaboration with Ben Evans of the University of Pennsylvania, discusses the risk management strategy behind Penn Medicine’s $1.5 billion hospital pavilion.

Nov 04, 2025

Oct 14, 2025

Jul 29, 2020

Jul 21, 2022
August 15, 2017
In this issue, The Graham Company discusses its unique, proactive approach to risk management, which has been serving clients in high-risk industries for more than 50 years. Producer Luke Foley explains management liability insurance, and the Risk Management Center tool and new headquarters renovations are highlighted.

Nov 04, 2025

Oct 14, 2025

Jan 24, 2022

Dec 17, 2020